There were 48 heart attacks on Bainbridge Island last Saturday — and all in the same location.
But that’s OK. It worked out as well as it could, because there was plenty of help around.
Plenty of highly qualified help.
Actually, if you were going to have a massive heart attack last weekend, Saturday, at the Bainbridge Island Fire Department’s Station 23 on Phelps Road, was kind of the ideal place to do it. That is because it was the site of the annual “Mega Code” drill session for the University of Washington’s Medic One paramedic training program. Twenty-four students from nine different departments, some from as far away as The San Juan Islands, converged on Station 23 for the big day, one of several such “field trips” they undergo throughout the 10-month program.
“Much of the learning is based on scenario-based training,” said BIFD Assistant Chief Luke Carpenter, one of the event’s primary organizers. “This event today is called Mega Code. They do other trips like this — to other departments, and places like Bellevue — to do things like mass casualty training and active shooter training to get out in the field and do field work.
“You can only learn so much in a classroom and you may not see it in your ridealongs in the medic units, so they come out and do days like this.”
Medic One is the program that BIFD paramedics go through as well, and though no Bainbridge-based students were among this year’s class specifically, the benefits of participating for the island department were many said BIFD firefighter/paramedic Kory Abercrombie, who was himself a student in the very same program just two years ago.
“It’s a growing and learning experience,” he said. “Our biggest thing is we get training for our guys, for our EMTs and firefighters. They get to do this routine over and over again, and we get to stay connected to a system that we send our paramedics through, kind of maintain that bond.”
By “the routine” he means CPR, because all though the students don’t know exactly what to expect when they walk into each of the four different scenarios, they all at least end the same way.
“There are four scenarios and each one will start out differently but winds up with the patient being in cardiac arrest,” Carpenter explained. “Maybe [it’s] drug overdose, maybe medical condition or this, that or the other thing. The long and short of it is: The patient winds up in cardiac arrest and the students have to deal with that.”
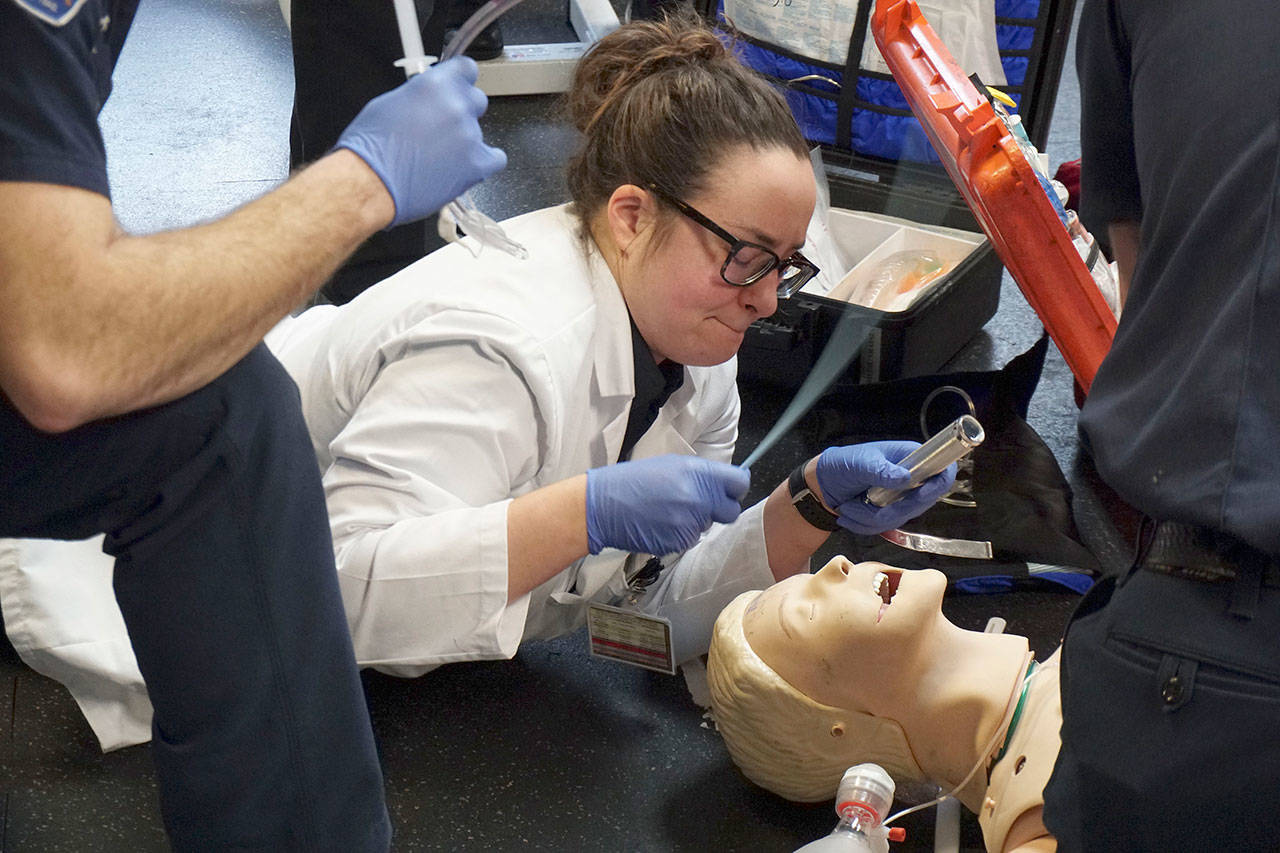
Sometimes students walk in to find an actor playing a soon-to-be-patient — “I can’t breathe,” “My chest hurts,” etc. — before moving on to the CPR dummy, or they may come in sans intro and find the collapsed “patient” on the floor and not responsive. Some are collapsed in the gym, others in offices or dorm rooms, and they all need help ASAP.
“We got dead people everywhere,” Carpenter said.
The response to such an incident — cardiac arrest — requires many hands; many well trained hands working together, Carpenter said.
“It’s a pretty amazing little ballet,” he explained. “The neat thing about the system here is the doctors and paramedics work so well together. It has to be that kind of a relationship to provide the best outcome for the patient, so it’s really nice that they’re involved in the training.”
Qualified paramedics are standing by, orchestrating the scenarios and advising the students as to the patient’s “symptoms” and “vitals,” so they can respond properly — or not — as well as actual doctors to supervise and critique.
“The students also have radios so they can call the doctors in the ER — which just happens to be out in the apparatus bay,” Carpenter said. “But we have Harborview doctors who’ve come over and are participating in this with us, so it’s as real as we can make it.
“When they deliver the patient to the ER, the doctors will critique them. And it’s great, because that’s what happens in real life,” he added. “That’s the beauty of it.”
Bainbridge firefighters are there to act as EMTs and, well, firefighters.
“In a normal response like this you’d have EMTs who respond with the paramedics, so our firefighters are working with the Seattle students, acting as their crews, their support teams, just as they would here,” Carpenter said. “We get to work with these guys under the guidance of doctors. It’s fantastic training for us because our guys and girls will go through 24 CPR scenarios today. Practice makes perfect, and they do it over and over again.”
Medicinal expertise is only part of the class’ goals, according to Dr. David Carlbom (who is director of the Michael K. Copass Paramedic Training Program and also associate professor of the Division of Pulmonary and Critical Care at the UW’s School of Medicine), one of the day’s training’s most crucial evaluators.
“That’s about a third of it,” he said, adding teamwork and leadership — “I’m really looking at how the students are communicating and leading their team.”
Add equanimity — “Will they stay calm with someone dying in front of you?” — to the list.
“Those are the three skills they really need to know,” Carlbom said. “The medicine is just a part of it.”
The biggest takeaway for a non-participant might just be the length of time responders spend with each patient. Carpenter said that, unlike on TV or in movies, CPR is not an immediate fix. The average resuscitation time is something like 20 to 40 minutes, in fact.
“It doesn’t take place during the commercials,” he said.
The BIFD has hosted at least one such joint training event annually for more than 20 years, according to Carpenter.
“We rotate through all the tasks that have to be done so everybody gets comfortable with it,” he said. “It doesn’t matter whether you’re a paramedic or you’re a firefighter; you’re all working as a single unit for the outcome.”